Rh Factor of a child
Rhesus (Rh) factor
The blood type is determined by molecules on the surface of red blood cells. If the red blood cells have antigen A, then you have blood group A. If antigen B is present, your blood group is type B. In the presence of both A and B antigens, your blood group is type AB. And in the absence of these antigens, you have blood group type O.
Rh factor is a protein that is also found on the surface of red blood cells. If this protein (antigen D) is in the blood, then you have a positive Rh factor (Rh +). If this protein is not in the blood, then the Rh factor is negative. Rh positive is the most common blood type.
Taking into account the blood group according to the ABO system, as well as the Rh factor, the main blood groups can be distinguished:
- O+, O-
- A+, A-
- B+, B-
- AB+, AB-
Pregnancy and Rhesus (Rh) Factor
The presence or absence of Rh factor in the blood does not affect health in any way. However, some problems can arise during pregnancy if the mother is Rh negative, and the baby is Rh positive.
If the baby's blood enters the mother's bloodstream, Rh antibodies may be produced in the mother's blood. These antibodies can enter the placenta and attack the baby's blood cells.
Usually, the baby's and mother's blood are only mixed during childbirth. Therefore, different Rh factors in mother and child are not a problem during the first pregnancy.
In addition to childbirth, other factors, such as bleeding during pregnancy, amniocentesis, miscarriage, ectopic pregnancy, can also cause the baby's blood to enter the mother's bloodstream.
Genetics
The Rh factor is inherited from parents. The child inherits a set of genes from the mother, and the same set from the father. As a result, each gene is present in two copies (alleles) passed down from each of the parents.
The allele that contains the D antigen (Rh+) is dominant. An allele that does NOT contain the D antigen (Rh-) is recessive. This means that if one person has two different alleles, then his Rh factor will still be positive, since the allele with the D antigen dominates over the allele in which this antigen is absent.
Conventionally, an allele with an antigen is denoted by a capital D, and an allele without an antigen is denoted by a small d.
For example, both the mother and father have a positive Rh factor. But each of them has different alleles responsible for the Rh factor. One allele contains the D antigen, while the other does not. One of the father's alleles and one of the mother's alleles can be transmitted to the child at random.
A simple Punnett square illustrates this example:
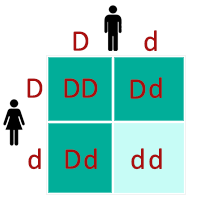
This means that in 75% of cases, the child will have a positive Rh factor, and in 25% of cases negative Rh factor. That is, even if both parents are Rh-positive, they may have a Rh-negative baby.
Blood Donation and Compatibility
Understanding blood types goes beyond just personal health. It's crucial for safe blood transfusions. People can only receive blood compatible with their ABO type and Rh factor. A mismatch can trigger a severe immune reaction, destroying the donated red blood cells. Knowing your blood type allows you to donate blood to those in need while ensuring safe transfusions when necessary.
The ABO and Rh systems are the most common classifications, but there are over 300 other blood group systems. These systems have less impact on blood transfusions but can be important in specific situations.
There are blood group antigens that can play a role in blood compatibility and transfusion reactions. These antigens, such as the Kell, Duffy, and Kidd antigens, among others, are less well-known but can be crucial in certain medical situations.
For example, the Kell antigen system consists of over 30 antigens, with the Kell antigen (K) being the most clinically significant. Antibodies to the Kell antigen can cause severe hemolytic disease of the newborn or hemolytic transfusion reactions. Similarly, the Duffy antigen, found on red blood cells, is important in blood transfusion and malaria susceptibility. Individuals who lack the Duffy antigen are resistant to Plasmodium vivax malaria.
Understanding these additional blood group antigens is essential in transfusion medicine and prenatal care. Incompatibilities between these antigens can lead to adverse reactions, so blood typing beyond the ABO and Rh systems is often necessary in certain medical contexts.
Moreover, advances in genetic testing have provided more detailed information about blood group genetics and inheritance patterns. With technologies like next-generation sequencing, healthcare providers can identify rare blood group variants and predict potential risks associated with transfusions or pregnancies.
In clinical practice, knowledge of blood group genetics enables healthcare professionals to provide personalized care to patients. For instance, in cases where blood transfusions are needed frequently, such as in patients with thalassemia or sickle cell disease, matching for additional blood group antigens beyond ABO and Rh can reduce the risk of alloimmunization and transfusion reactions.
Furthermore, understanding blood group genetics is vital in the field of organ transplantation. Matching for compatible blood groups between donors and recipients can improve the success rate of organ transplants and reduce the likelihood of rejection.
In summary, while the ABO blood group system and the Rh factor are fundamental in blood typing and compatibility testing, it's essential to recognize the role of other blood group antigens and advancements in genetic testing. This comprehensive understanding enhances patient care and safety in various medical scenarios, from transfusion medicine to organ transplantation.